Sudden Low Back Pain: What Helps, What to Avoid, and How to Support Recovery
Sudden low back pain is one of the most common reasons people seek care and one of the most mismanaged in those critical first few days.
One day you're moving normally. The next, getting out of bed feels like a project. For most people, the pain itself isn't the only problem. It's not knowing what to do first, what to avoid, or whether they're making things worse.
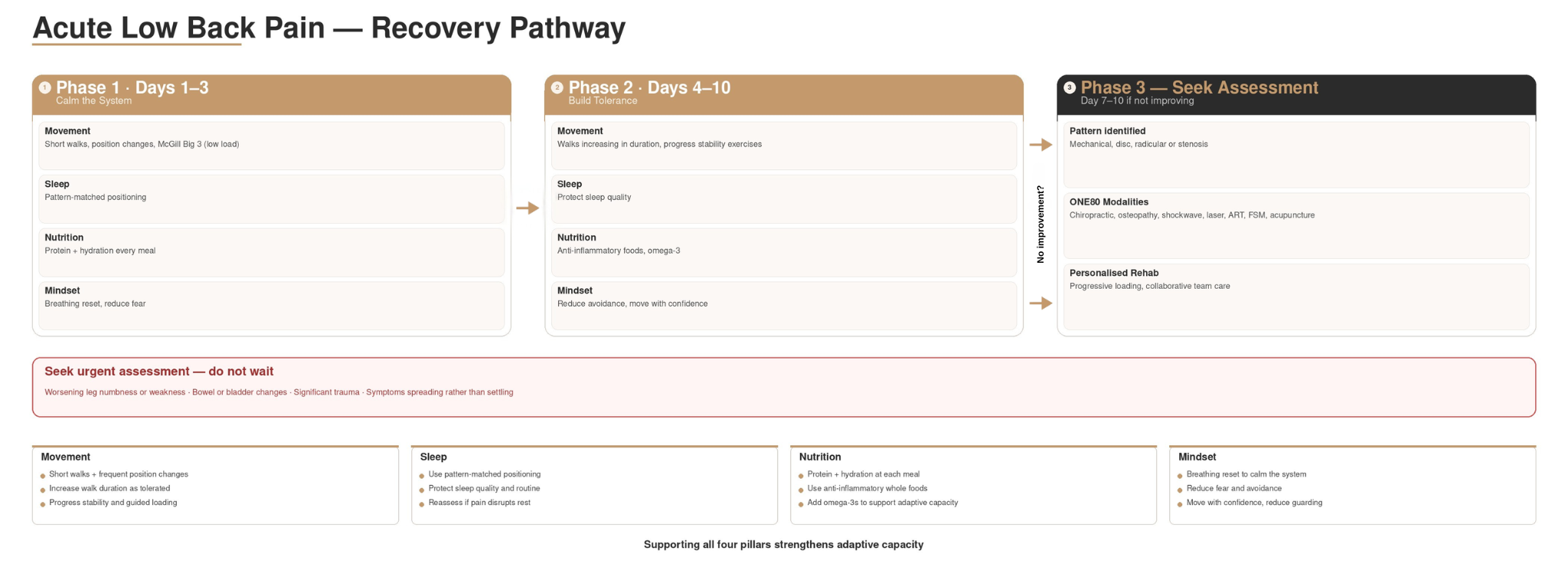
This guide covers what actually helps in the early days, organized around the Four Pillars of Health that guide our clinical approach at ONE80: Movement, Sleep, Nutrition, and Mindset.
Why Sudden Low Back Pain Happens
The lumbar spine is a load-bearing system built from joints, discs, muscles, ligaments, fascia, and nerves. It's designed to be both strong and adaptable but because it manages load continuously throughout the day, it's also vulnerable when demands exceed capacity.
Acute flare-ups commonly occur when:
Load exceeds tolerance - either from a single event or cumulative strain
Recovery is reduced - poor sleep, chronic stress, or under-fueling
Movement patterns become protective - guarding leads to stiffness and more sensitivity
Sometimes a specific structure is irritated: a disc, a facet joint, a muscle. In other cases, the nervous system itself becomes more sensitized, and pain feels louder than the actual tissue state warrants. Often it's a combination of both.
Understanding this matters because 'protect at all costs' is rarely the right response. The body usually recovers better with guided movement, not shutdown.
Common Low Back Pain Patterns
A proper assessment is needed for diagnosis. But most cases fit recognizable patterns and understanding your pattern helps you avoid one of the most common mistakes: doing a popular exercise that's wrong for your presentation.
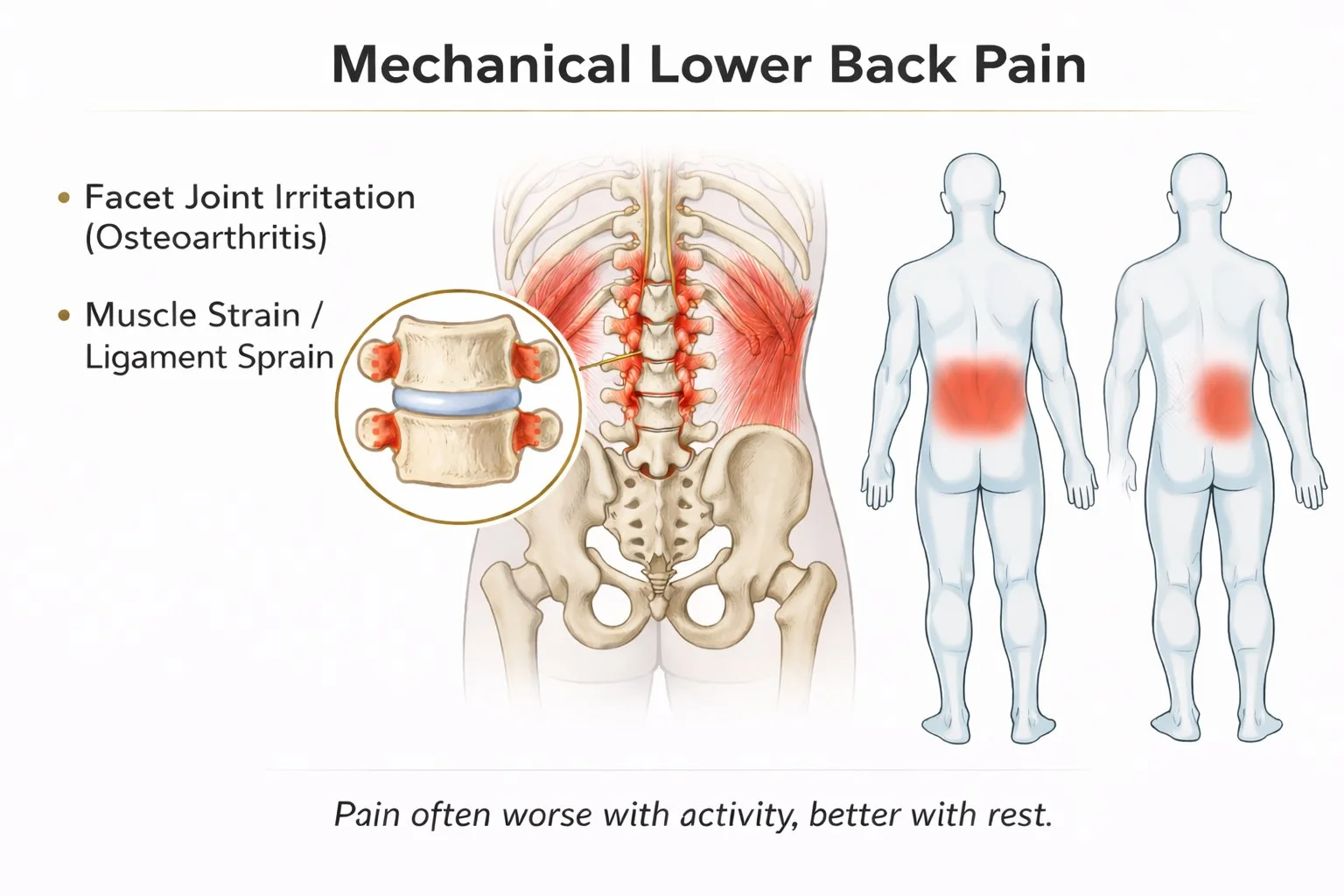
Mechanical / Axial Low Back Pain
Localized to the low back or buttock area
Position- or load-dependent (certain movements ease it, others aggravate)
Typically improves gradually with appropriate activity
Disc Irritation / Discogenic Pattern
Often worse with sitting or bending forward
May be sensitive to coughing or sneezing (increased disc pressure)
May include referred symptoms into the leg
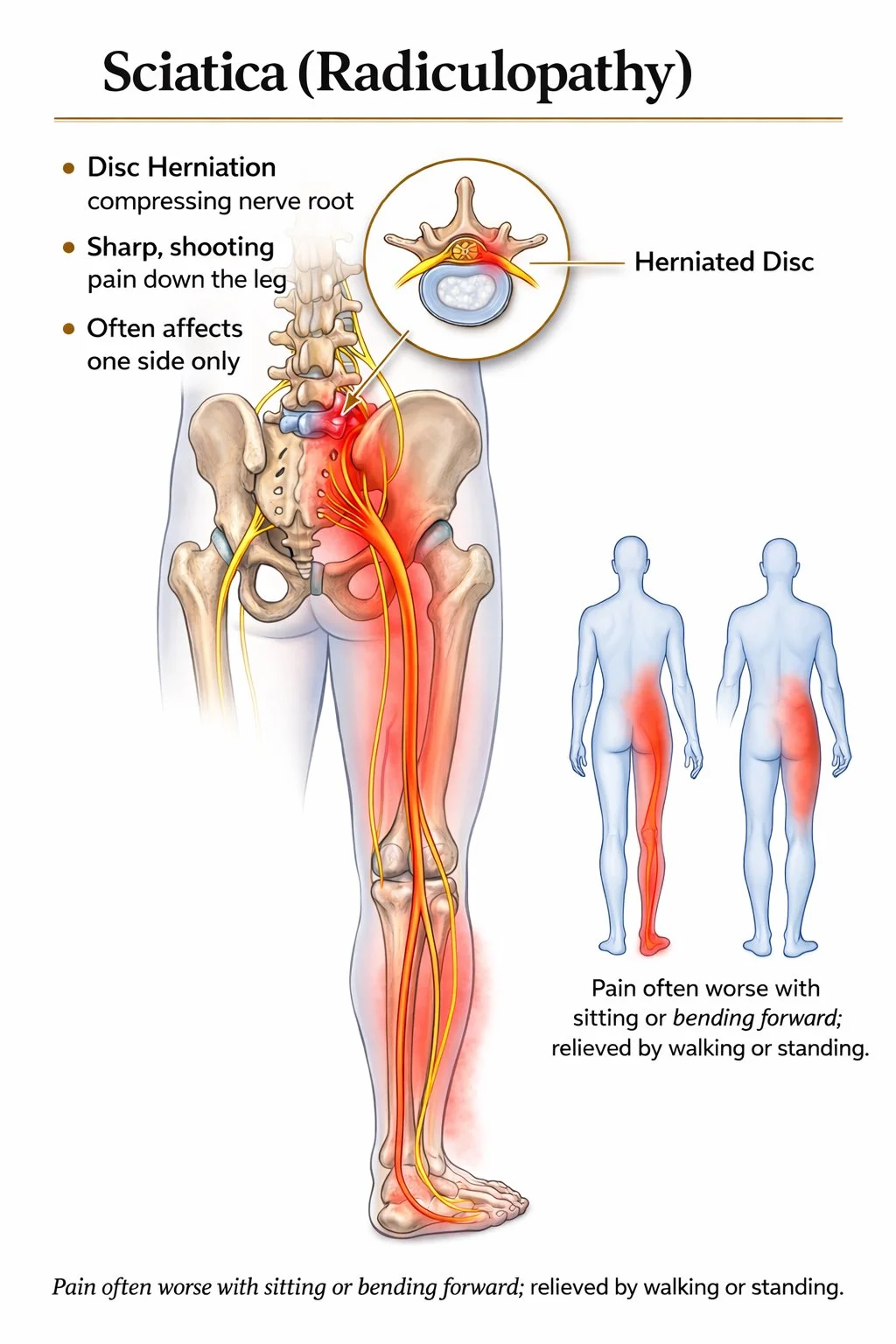
Sciatic / Radicular Pattern
Pain traveling into the buttock and down the leg
Burning, electric, or sharp sensations
Numbness or tingling in the leg or foot
Weakness warrants prompt assessment
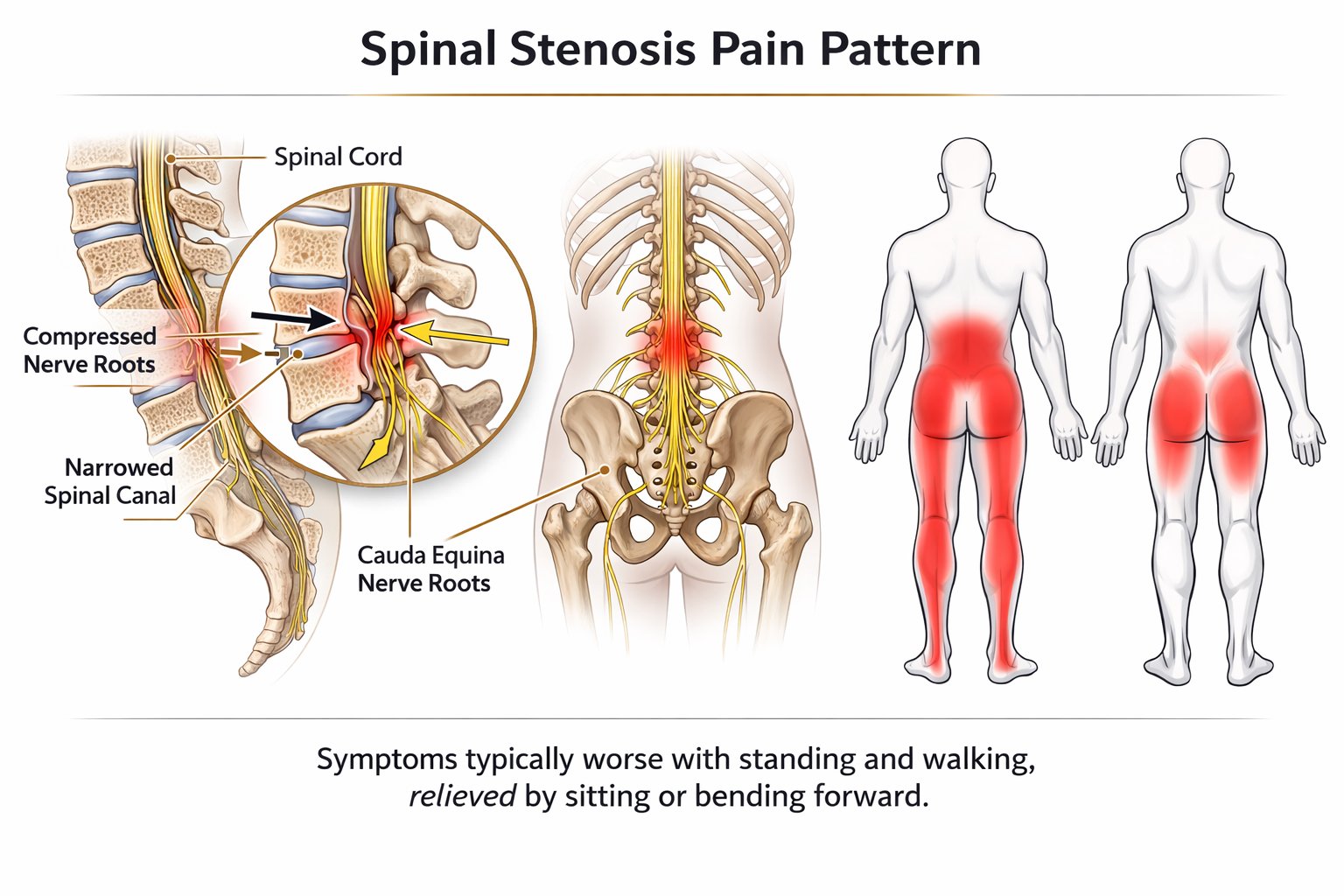
Stenosis Pattern
More common with age-related changes in the spine
Worse with standing or walking; relieved by sitting or bending forward
Heaviness or fatigue in the legs with sustained activity
These patterns overlap and can co-exist. If you're unsure, assessment clarifies which approach fits your situation.
What Helps vs. What Often Makes It Worse
What often slows recovery
Prolonged bed rest
Repeatedly testing painful movements
Aggressive stretching into pain
Heavy lifting or twisting too soon
Waiting weeks with no improvement
What tends to help
Gentle walking and regular position changes
Spine-sparing stability work
Adequate hydration and protein intake
Supportive sleep positioning
Slow breathing to calm the nervous system
Movement: Stay Active, Within Tolerance
One of the most damaging things you can do after sudden back pain is go to bed and stay there. Prolonged rest increases stiffness, amplifies pain sensitivity, and slows recovery. The goal isn't to push through pain, it's to stay gently active within comfortable limits.
Movement maintains circulation, reduces protective guarding, and signals the nervous system that it's safe to move.
What tends to help
Short walks, taken often
Frequent position changes; avoid staying in one position too long
Small, comfortable 'movement snacks' throughout the day
What often makes it worse
Staying in bed for more than a day
Forcing stretches or exercises into pain
Heavy lifting or twisting before symptoms settle
Foundational Stability Exercises (McGill-Inspired)
These three exercises target deep spinal stabilizers with minimal load. They are done as short holds, not to fatigue. Stop if symptoms worsen.
Bird Dog
From hands and knees, extend opposite arm and leg
Hold 5-8 seconds - 4 to 5 reps per side
Keep spine neutral throughout
Modified Curl-Up
On your back, one knee bent, hands under the lower back
Lift only head and shoulders slightly - hold 5-10 seconds
5 reps - do not perform a full sit-up
Modified Side Plank
Knees bent, propped on forearm
Hold 5-10 seconds - 3 to 5 reps per side
Progress to straight-leg only when comfortable
These should feel steady and controlled; never painful or fatiguing. Tip: aim for quality of position, not duration.
When Extension May Help: The Prone Press-Up
Some back pain patterns feel significantly worse with sitting or bending forward. In those cases, a gentle extension movement can provide relief not always, but often enough to be worth trying.
Prone Press-Up:
Lie on your stomach on a firm surface
Place hands under your shoulders
Slowly press your chest upward while hips stay relaxed and on the floor
Move only into a comfortable range; no forcing
Repeat 5-8 times
If symptoms spread further down the leg or worsen, stop and get assessed. Not every pattern responds to extension.
Sleep: Positioning Based on Your Pattern
Pain frequently feels worse at night during a flare-up. Disrupted sleep raises pain sensitivity the next day, creating a cycle that prolongs recovery. Positioning can reduce tension in the low back and make rest more accessible.
If Sitting or Bending Forward Increases Pain
(Often associated with disc-related patterns)
Try lying on your back with a pillow under your knees
Or briefly lying on your stomach before sleep, if that feels comfortable
If Standing or Walking Increases Pain
(Often associated with stenosis-type patterns)
Try side sleeping with a pillow between your knees
Allow a slight bend at the hips and knees
These are acute-phase comfort strategies, not permanent sleep habits. Once the flare settles, return to your normal position. If sleep is consistently disrupted or symptoms persist, assessment helps target the right approach.
Nutrition: Fuel Recovery, Don't Neglect It
When pain arrives, appetite and routine often drop off. But this is exactly when the body needs consistent energy and nutrients to adapt and repair. Under-fueling slows recovery and may amplify pain sensitivity.
Foundation Habits
Stay well hydrated throughout the day (urine should be pale yellow)
Eat regular meals; do not skip, especially protein
Include a quality protein source at each meal
Favour whole, minimally processed foods during the flare
Evidence-Informed Nutrients (Optional, Not Essential)
These are not required for recovery, but some patients find them helpful during a flare-up. Doses below reflect ranges used in research literature and common supplement labelling, always check with a regulated health professional if you take medications or have existing conditions.
Omega-3 Fatty Acids (EPA + DHA)
Supports inflammation regulation
Research commonly references ~1.35-2.7 g/day of combined EPA+DHA in chronic pain literature
Caution: consult a clinician if you take blood thinners or are planning surgery
Magnesium
Supports muscle relaxation and sleep quality
Clinical trials show benefit for insomnia in certain populations
Caution: check with a clinician if you have kidney disease or take certain medications
Curcumin / Turmeric Extract
Supports the inflammatory response - RCT use in musculoskeletal conditions typically 500 mg twice daily of standardized extract
Caution: gallbladder issues, reflux, or antiplatelet medications, consult a clinician first
Collagen Peptides + Vitamin C
Connective tissue support, research suggests 5-10 g/day collagen with vitamin C
Most effective when paired with progressive loading (rehab)
Supplements are individualized. If you are pregnant, breastfeeding, on medications, or have kidney or gallbladder conditions, consult a qualified clinician before starting any supplement.
Mindset: Reduce Threat, Reduce Tension
Sudden pain almost always triggers fear: Is this going to get worse? Did I do something to cause this?
Fear increases guarding, avoidance, and pain amplification. It leads many people to stop moving which, as we've covered, typically makes things worse. Understanding a few key points can change the trajectory of recovery significantly.
Acute low back pain is not always a sign of serious damage. In many cases, it reflects how the body is responding to accumulated stress, fatigue, or overload; not a structural failure.
Pain is a protective signal, not a damage report. The nervous system can amplify pain well beyond what the tissue state warrants, especially under stress or fear.
3-Minute Breathing Reset
Slow breathing reduces sympathetic nervous system drive which directly reduces protective muscle tension. This isn't psychological; it's physiology.
Inhale through your nose for 4 seconds
Slowly exhale for 6-8 seconds
Repeat for 10-15 breaths
Calm understanding increases movement confidence. Movement confidence accelerates recovery.
When to Seek Assessment
Most episodes of acute low back pain improve within days to weeks when managed well. However, waiting too long without improvement is a common reason recovery stalls.
General guideline: if symptoms are not clearly improving within 7–10 days, get assessed. The earlier a clear pattern is identified, the faster the right approach can be applied.
Seek Assessment Sooner If:
Symptoms are worsening rather than stabilizing
Pain is radiating with progressing numbness or weakness in the leg
Significant trauma occurred (fall, motor vehicle accident)
Bowel or bladder changes have occurred, this requires urgent assessment
Summary: The Four Pillars in Practice
Movement: Short walks, frequent position changes, McGill-style stability work, within tolerance
Sleep: Pattern-matched positioning strategies to reduce tension and protect sleep quality
Nutrition: Protein + hydration + whole foods as the foundation; optional evidence-informed nutrients for flare support
Mindset: Reduce fear; calm the nervous system; breathe and move within tolerance
Supporting these pillars strengthens resilience and adaptive capacity, the body's fundamental ability to respond to stress and return to balance.
Not improving after 7–10 days?
Our team can assess what's driving the pain and build a plan tailored to your pattern. Same-day and next-day appointments available.
FAQ
-
In most uncomplicated cases, gentle movement helps more than prolonged rest. Rest has its place in the first 24–48 hours, but beyond that, staying active within comfortable limits speeds recovery and prevents stiffness from compounding pain.
-
No. Many cases are mechanical or sensitivity-dominant, with no structural disc involvement. Patterns overlap and a proper assessment not assumptions, should guide the approach.
-
If symptoms aren't clearly improving within 7–10 days, or if they're worsening, it's wise to get assessed early. If nerve symptoms (numbness, weakness, radiating pain) are progressing, seek care sooner. Bowel or bladder changes require urgent attention.
-
It depends on the pattern. The safest early starting point for most people is low-load stability work (bird dog, curl-up, side plank) combined with walking and frequent position changes. Avoid high-intensity or pain-provocative exercises until symptoms settle and a pattern is identified.
-
Many episodes improve significantly within a few days to two weeks when managed appropriately. The quality of what you do in the first week matters more than most people realize.
Disclaimer
This article is for educational purposes only and is not intended to provide medical advice, diagnosis, or treatment. Individual situations vary and should be guided by a qualified healthcare professional.